I wish that title were tongue-in-cheek, but I tweaked my right knee last week, and for the last few days I’ve been resting my legs while the swelling goes down. It’s feeling better, and I’m pretty sure I’ll be able to run again by the weekend, but in the meantime, I’m feeling proud of myself for not running through an injury, however mild it might be.
After the gauntlet of appointments with my gyn onc, medical oncologist, and surgeon, I’m now in that grey zone of waiting for my first infusion to be scheduled.
If you’re new here, I’m navigating not one, but two, cancers—colorectal and endometrial. One body, two primaries, zero chill from my cells apparently.
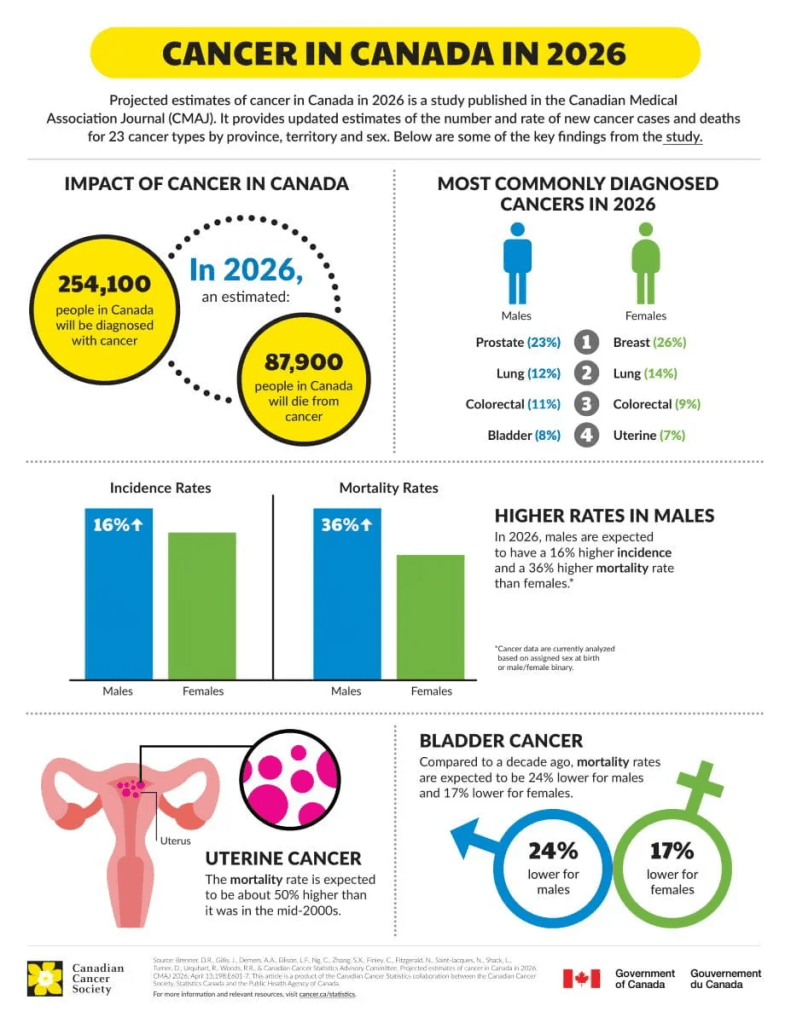
The Canadian Cancer Society released its 2026 cancer statistics this past Monday, and according to the new report, I’ve managed to land on #3 and #4 on the list of most common cancers in Canadian women. Overachiever, that’s me.
The only appointment I had this week was with the pivot nurse for my surgery. She was warm and engaging, answering all my questions and clearly patient-focused. I left knowing how my surgery would unfold, and having agreed to be her patient partner in updating the booklets that the hospital gives you to prepare for your procedure.
Eat the rainbow … or not
It’s not surprising that surgery to remove a significant portion of your digestive system will require some diet adaptations post-surgery. It’s not dissimilar to what I went through during radiation treatment. I call it my ‘white diet’ since low-fibre, low-residue means white bread, white rice, eggs, apple sauce, etc. For the first two weeks, the goal is to hit my protein targets, likely with supplements like my protein powder, while restricting the amount of roughage to digest, so that my new configuration has time to heal.
From there, I’ll be able to reintroduce colours on a gradual timeline, testing how my body handles this new system, and hoping that the adaptation means I don’t have to give up favourites.
Because I’m having a robotic procedure, the new connection between my colon and small bowel will be done internally, and that means a faster recovery and much smaller incisions than open surgery. I should be about two days in hospital, assuming my digestive system cooperates and signals its readiness in the way that post-surgical systems are apparently required to do before you’re allowed to go home. Trust me, you don’t want those details. The indignities are many, but they are finite.
Sitting with uncertainty
What’s harder to prepare for is the treatment that comes before surgery — two cycles of immunotherapy, the first of which likely means an overnight hospital stay for monitoring. The potential side effects are well-documented and genuinely variable—you can read the list, talk to your oncologist, do all the research, and you still can’t know in advance which ones, if any, will show up for you personally. That particular uncertainty—informed but unresolved —is its own kind of anxiety. It’s a bit like prepping for a new race distance—you can do the work, you can test your fitness, but until you toe the line, you won’t know what the experience feels like, or how your body will absorb the effort and recover afterwards.
I’m not someone who does well with waiting. My instinct is to research, prepare, optimize, and track. I’ve done all of that. But there’s a point at which the preparation is complete, and what remains is just the waiting—for the infusion date, for the first treatment, for whatever my body decides to do with it.
What I’m giving up, and what I’m not
I had hoped to run a 10k or a half-marathon this fall. That’s off the table now, and I’m not going to pretend that’s a small thing. If you organise your year around race seasons, you know: losing a fall target isn’t just a scheduling inconvenience — it’s a real shift, a recalibration of what the next several months are for.
But I’m not giving up movement. It’s non-negotiable, and it’s not bravado. Going through chemo, the days I ran or walked were better than the days I didn’t. Not because I felt good, but because moving reminded me that my body was still mine and still capable of something. Radiation was the same. Parcelling the Toronto Marathon into 2.6-mile increments gave me a different way to navigate the treatment timeline, and running the final leg on race day, close to when I finished, let me know I could still do hard things — even if they followed a different path. I expect this treatment cycle to be no different.
So the goal has shifted from racing—some weeks will mean actual running, some will be a walk around the block. And as different as that looks, summer in Montréal, on the mountain or by the canal, is a great season to be outside. The forecast is for 19°C and sunny on Saturday, so after this week’s dreary weather, I may find myself on the mountain for the first time this spring.
That fall race will have to wait for me.
Postscript: In the time between writing this and pressing publish, everything changed. A colleague of my medical oncologist called just now with news. The tumor board met today, and the decision is that immunotherapy is off the table. My tumor is small enough, and my other CT findings unrelated enough, that the treatment plan has been simplified considerably. Surgery is now scheduled for next Friday.
Complicated feelings doesn’t begin to describe what comes with good news delivered as a radical change of plans. That will need its own post. For now, the waiting game I described above just got a lot shorter.
Leave a comment